Bernard-soulier syndrome is a bleeding disorder where the affected individuals are presented with abnormal size and low quantity of platelets. These platelets are essential for blood clotting process. The cases of the bernard-soulier syndrome have problems with the platelets which do not stick together properly to the blood vessel wall during an injury making it difficult for the normal process of blood clotting to form. Hence, these individuals tend to bleed excessively after an injury and may also bruise easily. The prevalence of this syndrome is estimated to affect 1 in a million individuals, however, research suggests that the condition may be more common as many cases remain under-diagnosed.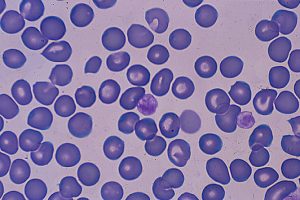
Symptoms
The symptoms of bernard-soulier syndrome vary from one affected individual to another. In most cases, the symptoms are evident at the birth of the infant and continue throughout their life. In some cases, the symptoms do not occur until their adult life. This includes the excessive bleeding from injuries, nosebleeds, and heavy menstrual period in women. In addition, they may bleed from the gums, abnormal bleeding after a surgery and rarely vomit or excrete blood in the stool as the result of internal bleeding in the stomach.
Causes
Bernard-soulier syndrome develops as the result of the mutation in one of the three genes: GP1BA, GP1BB or GP9. These genes are responsible for the production of a certain protein complex called glycoprotein (GP) Ib-IX-V present on the surface of platelets that play an essential role in blood clotting. The mutation in one of the three genes prevents the formation of the protein complex on the surface of the platelets. This impairs the clot formation resulting in the excessive bleeding episodes associated with this condition.
This syndrome is inherited in an autosomal recessive pattern where both the copies of GP1BA, GP1BB or GP9 in each cell are defective. The parents of autosomal recessive pattern disorder each carry one copy of the defective gene and usually do not show any symptoms associated with this condition, although some may exhibit mild bleeding abnormalities.
In rare cases, GP1BA or GP1BB are inherited in an autosomal dominant pattern where one copy of the defective gene is sufficient to cause this syndrome.
Diagnosis
The diagnosis is based on a thorough assessment of the individual’s medical history and with various laboratory tests. The blood test can reveal the presence of large, irregularly shaped and abnormally low level of platelets. The biochemical tests can detect the efficiency of platelets to start the clotting process. The molecular genetic test can identify the mutated gene that is responsible for the cause of this syndrome.
Treatment
The treatment for these cases is only required during surgical procedures, dental work or after an injury. In the case of severe bleeding episodes, platelet transfusion can treat the condition. These individuals should refrain from taking medications such as aspirin as this can affect the clotting process. They may take acetaminophen medications such as tylenol for the pain relief. Women may be administered hormonal contraceptives to control the excessive menstrual bleeding. Antifibrinolytic agents are usually used to reduce the bleeding after surgery, dental work and prolonged nosebleeds. Iron replacement may be required to treat anemia which may develop from excessive bleeding episodes.



